What is APDS?
APDS is a progressive, underdiagnosed primary immunodeficiency (PI)1-3
DIAGNOSING APDS
APDS has been diagnosed as another PI or condition, causing delays in diagnosis4
Of 39 patients who had an initial clinical diagnosis other than APDS5:
Adapted from Jamee M, Moniri S, Zaki Dizaji M, et al. Clinical, immunological, and genetic features in patients with activated PI3Kδ syndrome (APDS): a systematic review. Clin Rev Allergy Immunol. 2020;59(3):323-333.
APDS can result in permanent organ damage and increased mortality risk. The median age of death was 11 years earlier than the general population (64 years vs 75 years).3,6,7
A genetic test can help inform a diagnosis of APDS
Recognizing the symptoms of APDS and conducting genetic testing are crucial for diagnosing and managing the condition4,8
IMPACT OF DELAYED DIAGNOSIS
Seemingly common symptoms may signal underlying immune deficiency and dysregulation3,5
Timeline of most common pathologies seen in APDS5,8-10
Genetic testing can help inform a diagnosis of APDS for patients and their families4,8
- Because APDS is an autosomal-dominant, inherited condition, family members of individuals with APDS should consider genetic testing, including parents, siblings, grandparents, aunts, uncles, and cousins.
There is a 50% chance of APDS being passed down from parent to child11-13
- Consider testing for APDS if presented with any of these clinical features5:
- Previously treated with mTOR inhibition or other immunosuppressants
- Elevated IgM levels
- Herpes virus infections
- Bronchiectasis
- Non-Hodgkin lymphoma
Missing these common pathologies may result in delayed diagnosis4
SUSPECTING APDS
Recognize atypical immune symptoms that may indicate APDS3,5,13-15
If you suspect PI, genetic testing can help inform an accurate diagnosis. Even a limited number of visible symptoms may indicate APDS.
People with APDS usually experience 1 or more of the following symptoms:
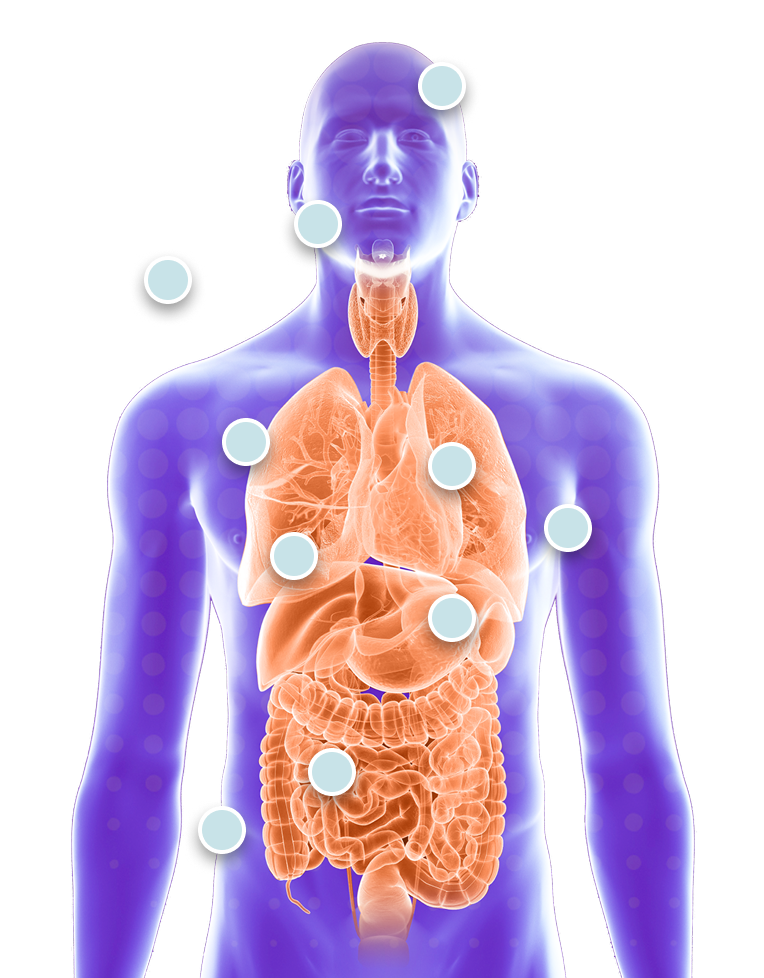
Children with APDS may present with symptoms differently.
IMPORTANCE OF GENETIC TESTING
If you suspect your patient may have a PI, genetic testing that includes the genes that cause APDS can help inform a timely diagnosis
Sponsored genetic testing option and genetic counseling are available for eligible patients and their families, regardless of insurance coverage or financial need

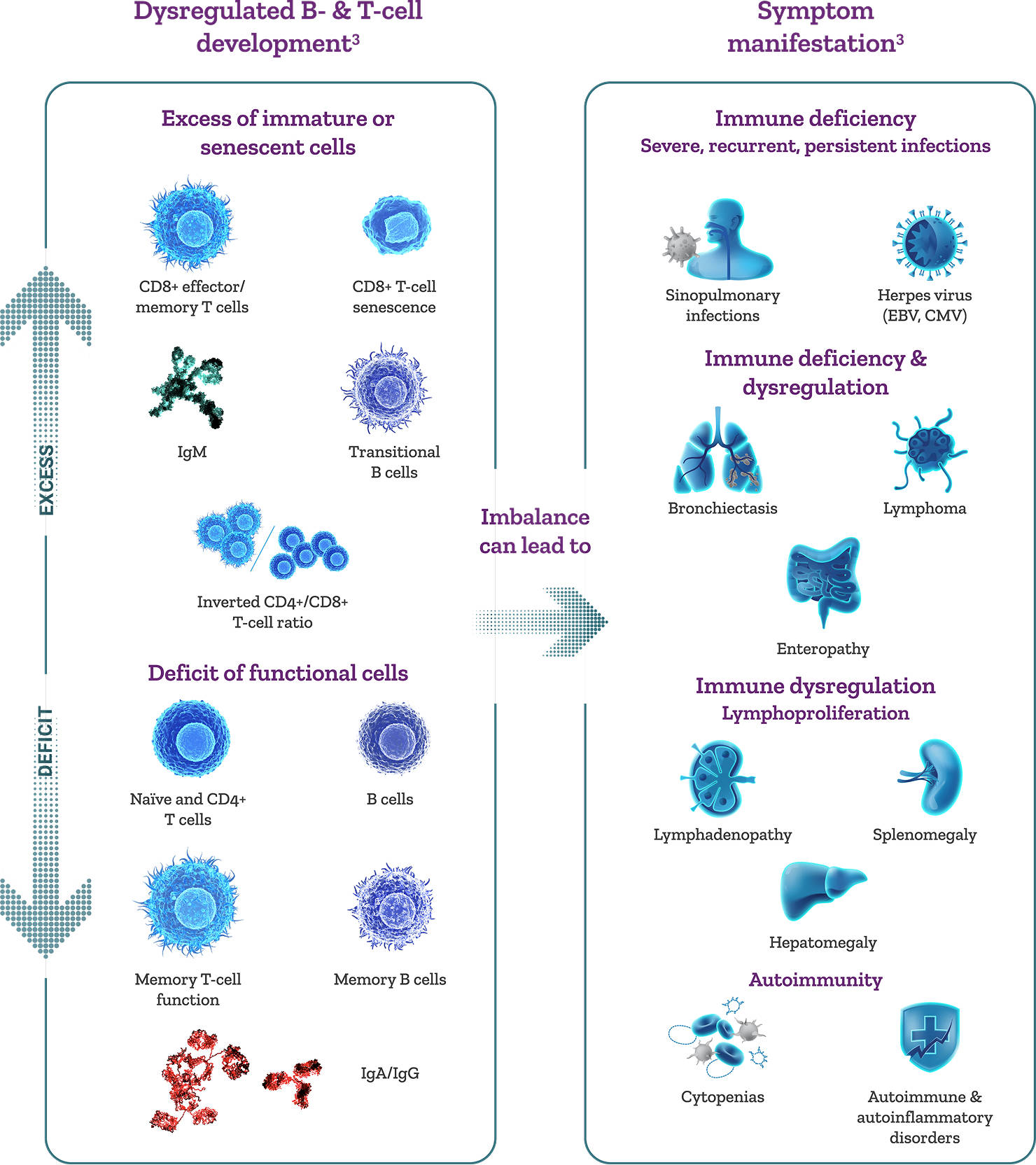
IMMUNE IMBALANCE IN APDS
A hyperactive PI3Kδ pathway drives immune deficiency and dysregulation responsible for APDS symptom manifestation3
- Uncontrolled immune dysregulation and deficiency may result in severe lymphoproliferation, recurrent infections, autoimmune disorders, and lymphoma3
- Lymphoproliferation can be a manifestation of immune dysregulation and can be associated with an increased risk of lymphoma3
Newer genetic panels now include APDS. If genetic testing was done prior to 2018 and your patient has symptoms of APDS, consider retesting.
How Joenja Works
→
APDS Assist
→
ALPS, autoimmune lymphoproliferative syndrome; APDS, activated PI3Kδ syndrome; CID, combined immunodeficiency; CMV, cytomegalovirus; CVID, common variable immunodeficiency; EBV, Epstein-Barr virus; IgA, immunoglobulin A; IgG, immunoglobulin G; IgM, immunoglobulin M; mTOR, mammalian target of rapamycin; XLA, X-linked agammaglobulinemia.
References: 1. Rao VK, Webster S, Šedivá A, et al. A randomized, placebo-controlled phase 3 trial of the PI3Kδ inhibitor leniolisib for activated PI3Kδ syndrome. Blood. 2023;141(9):971-983. doi:10.1182/blood.2022018546 2. Angulo I, Vadas O, Garçon F, et al. Phosphoinositide 3-kinase δ gene mutation predisposes to respiratory infection and airway damage. Science. 2013;342(6160):866-871. doi:10.1126/ science.1243292 3. Rao VK, Webster S, Šedivá A, et al. A randomized, placebo-controlled phase 3 trial of the PI3Kδ inhibitor leniolisib for activated PI3Kδ syndrome. Supplemental. Blood. 2023;141(9):971-983. doi:10.1182/blood.2022018546 4. Data on file. Pharming Healthcare, Inc. 5. Jamee M, Moniri S, Zaki-Dizaji M, et al. Clinical, immunological, and genetic features in patients with activated PI3Kδ syndrome (APDS): a systematic review. Clin Rev Allergy Immunol. 2020;59(3):323-333. doi: 10.1007/s12016-019-08738-9. PMID: 31111319 6. Rao VK, Kulm E, Šedivá A, et al. Interim analysis: open-label extension study of leniolisib for patients with APDS. J Allergy Clin Immunol. 2024;153(1):265-274.e9. doi: 10.1016/j.jaci.2023.09.032 7. Mahendran M, Upton JEM, Ramasubramanian R, Memmott HL, et al. Overall survival among patients with activated phosphoinositide 3-kinase delta syndrome (APDS). Orphanet J Rare Dis. 2025;20(1):212. doi: 10.1186/s13023-025-03734-z 8. Coulter TI, Chandra A, Bacon CM, Babar J, et al. Clinical spectrum and features of activated phosphoinositide 3-kinase δ syndrome: a large patient cohort study. J Allergy Clin Immunol. 2017;139(2):597-606.e4. doi: 10.1016/j.jaci.2016.06.021 9. Elkaim E, Neven B, Bruneau J, et al. Clinical and immunologic phenotype associated with activated phosphoinositide 3-kinase δ syndrome 2: a cohort study. J Allergy Clin Immunol. 2016;138(1):210-218.e9. doi:10.1016/j.jaci.2016.03.022 10. Maccari ME, Abolhassani H, Aghamohammadi A, et al. Disease evolution and response to rapamycin in activated phosphoinositide 3-kinase δ syndrome: European Society for Immunodeficiencies-Activated Phosphoinositide 3-Kinase δ Syndrome Registry. Front Immunol. 2018;9:543. doi:10.3389/fimmu.2018.00543 11. Michalovich D, Nejentsev S. Activated PI3 kinase delta syndrome: from genetics to therapy. Front Immunol. 2018;9:369. doi: 10.3389/fimmu.2018.00369 12. Lucas CL, Kuehn HS, Zhao F, Niemela JE, et al. Dominant-activating germline mutations in the gene encoding the PI(3)K catalytic subunit p110δ result in T cell senescence and human immunodeficiency. Nat Immunol. 2014;15(1):88-97. doi: 10.1038/ni.2771. 13. Sacco K, Uzel G. Activated PI3K delta syndrome. 2025 Jan 30. In: Adam MP, Bick S, Mirzaa GM, Pagon RA, Wallace SE, Amemiya A, eds. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993–2026. 14. Anderson JT, Cowan J, Condino-Neto A, et al. Health-related quality of life in primary immunodeficiencies: impact of delayed diagnosis and treatment burden. Clin Immunol. 2022;236:108931. doi:10.1016/j.clim.2022.10893 15. Ahmad Shawaludin MQ, Zainudeen ZT, Taib F, et al. A rare case report of activated PI3K delta syndrome (APDS): diagnostic pitfalls. BMC Pediatr. 2025;25(1):898. doi: 10.1186/s12887-025-06286-0